
Six things to help you get back on your feet quickly
Total hip replacement and total knee replacement are among the most successful surgeries performed today. For patients with severe hip or knee arthritis, total joint replacement can have a dramatic impact on quality of life by relieving pain and improving function, with excellent long-term results. In past decades, joint replacement surgery was commonly associated with a prolonged hospitalization and slow recovery. However, in recent years, modern techniques have evolved with a focus on minimizing the physiologic impact of surgery and facilitating a faster, easier recovery.
Increasingly, it is recognized that the majority of patients undergoing elective joint replacement are in reasonable health and can thus be managed with more preventive measures and less invasive monitoring and treatment. With appropriate preventive care and preparation for surgery, most patients can be treated according to a “well patient” model.
Current protocols for rapid recovery represent a new way of thinking about joint replacement surgery. Traditional models emphasized intensive hospital and institutional management of patients around the time of surgery because patients were treated according to a “sick patient” model. Treatment was reactionary rather than pre-emptive. Increasingly, it is recognized that the majority of patients undergoing elective joint replacement are in reasonable health and can thus be managed with more preventive measures and less invasive monitoring and treatment. With appropriate preventive care and preparation for surgery, most patients can be treated according to a “well patient” model, where the goals are to prevent common pitfalls and minimize the physiologic strain associated with joint replacement.
Preventive care in joint replacement focuses on avoiding the most common barriers to early mobility and recovery after surgery. In particular, rapid recovery protocols aim to reduce:
- Blood loss
- Dehydration
- Nausea
- Pain
- Limited mobility
- Inadequate education and planning
Modern protocols have been developed to combat each one of these issues and to limit the potential impact they might have. The result has been a major reduction in the length of time patients typically need to be in the hospital after surgery.
Limiting blood loss
Modern surgical approaches focus on minimizing trauma to the soft tissues and, in particular, avoiding muscle damage that can be associated with increased bleeding. Anesthesia can also reduce blood loss by helping to control intra-operative blood pressure. In addition, the use of tranexamic acid, an intravenous medication originally utilized to reduce bleeding in dental surgery, has been extensively studied in joint replacement surgery and shown to reduce blood loss and the need for transfusions without significantly increasing the risk of blood clot. Perioperative use of tranexamic acid in select patients has thus become common practice in many institutions.
Staying hydrated
 Dehydration after surgery can contribute to nausea, lightheadedness, and dizziness that can impair one’s ability to participate actively in early physical therapy. Traditionally dehydration was common since protocols suggested patients remain NPO, meaning having nothing to eat or drink, after midnight. The reason for these guidelines was to ensure an empty stomach to avoid anesthesia-related complications. However, new guidelines suggest that clear water can be ingested up to two to three hours prior to surgery. Reducing the amount of time patients go without drinking water and also ensuring appropriate intravenous fluid administration around the time of surgery can make a significant impact on patient hydration and can reduce the stress induced by the surgery.
Dehydration after surgery can contribute to nausea, lightheadedness, and dizziness that can impair one’s ability to participate actively in early physical therapy. Traditionally dehydration was common since protocols suggested patients remain NPO, meaning having nothing to eat or drink, after midnight. The reason for these guidelines was to ensure an empty stomach to avoid anesthesia-related complications. However, new guidelines suggest that clear water can be ingested up to two to three hours prior to surgery. Reducing the amount of time patients go without drinking water and also ensuring appropriate intravenous fluid administration around the time of surgery can make a significant impact on patient hydration and can reduce the stress induced by the surgery.
Preventing nausea
Getting up and moving can be particularly difficult if you are feeling queasy or sick to your stomach. The causes of nausea after surgery can include dehydration, general anesthetics, opioid pain medications, or simply eating too much too soon. As such, efforts to reduce nausea focus on appropriate hydration, limiting inhaled anesthetics, reducing the need for opioid pain medications, and providing appropriate anti-nausea medications. Identifying patients at high risk for nausea can also be helpful since some anti-nausea medications, including scopolamine patches and dexamethasone, can be given pre-emptively before the nausea occurs. Patients with a history of post-operative nausea, motion sickness, or nausea after narcotic pain medication, may particularly benefit from these preventive measures.
Limiting or managing pain
The management of pain after joint replacement surgery is the cornerstone of rapid recovery. Less pain means better ability to get back on your feet and get moving again. While some pain after surgery is certainly normal, the ability to limit that pain is critical if a patient is to mobilize effectively.
Traditional methods for pain control were focused primarily on narcotic pain medication, typically intravenous in the early post-operative period and transitioning to oral opioids during the hospital stay. While opioids are potent medications for managing pain, they have a myriad of side effects that run counter to the goals of rapid recovery. Excessive opioid use can result in nausea, fatigue, confusion or mental cloudiness, constipation, and itching. Furthermore, opioids can be habit-forming and, with prolonged use, increased opioid tolerance and increased pain sensitivity can be seen, which may result in a need for even higher doses of medication and thus a higher incidence of side effects.
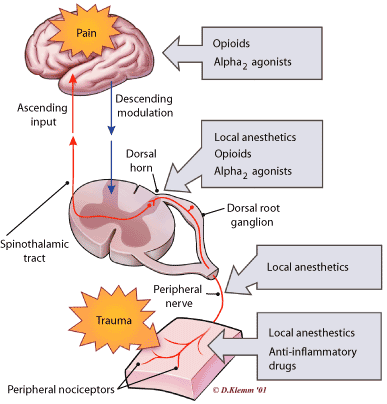
Redrawn with permission from Kehlet H, Dahl JB. The value of “multimodal” or “balanced analgesia” in postoperative pain treatment. AnesthAnalg 1993;77:1049.
Modern pain control regimens utilize what is referred to as “multi-modal analgesia” which essentially means that several different types of pain medications are used to block pain signals at various points along the pathway to the brain. Medications with different mechanisms of action can reduce pain in different ways and thus have a synergistic effect, meaning that the medications can work together so that the combined effect is greater than the sum of their individual effects. In this approach, the dose of any one medication can be relatively low and the side effects can be limited.
Whereas traditional pain control was reactive, modern pain control is pre-emptive. Before surgery, during the procedure, and after the surgery is complete, consistent efforts are made to prevent and reduce pain. Prior to surgery, a number of medications can be given in the holding area before the patient is ever taken to the operating room. These may include anti-inflammatory medications, nerve stabilizing medications, and low-dose long-acting opioids. Next, peripheral nerve blocks, spinal/epidural anesthesia, and/or local anesthetic injections can be useful techniques to reduce the pain signals generated during the surgery itself. Finally, multi-modal pain control regimens focus on consistent administration of scheduled non-narcotic pain medications that reduce the need for opioids and in some cases eliminate the need altogether.
Getting back on your feet
With the above measures in place, patients are better able to participate with physical therapy soon after surgery. By avoiding the other pitfalls, the primary focus in the immediate post-operative setting can be on teaching you how to get moving with your new joint replacement. While traditional protocols emphasized resting in bed early after surgery, today there is increasing recognition of the benefits of early mobilization and rehabilitation. Patients are typically able to get up and walk on the day of surgery or early the following morning. The sooner the therapy begins, the sooner you can get back to a level of mobility that will allow you to successfully get around at home.
Patient education and pre-operative planning
Rapid recovery after joint replacement ultimately hinges on the patient. Information is key and having a clear understanding of what to expect and how to plan for your post-operative recovery gives you the tools you need to be successful. With modern protocols, the amount of time patients spend in the hospital after surgery is steadily declining, such that one or two day stays are the norm and same-day discharge is increasingly feasible. Furthermore, with more patients able to discharge to home rather than rehab facilities, the risk of post-operative infection is reduced and patients are able to get back to their normal lives sooner than ever.
 Dr. Benjamin McArthur is a fellowship-trained orthopedic surgeon at Washington Orthopaedics & Sports Medicine. His specializations include hip and knee replacement, complex revision hip and knee replacement, and hip preservation surgery. He has published numerous peer-reviewed articles and has presented at national and international events on topics related to hip and knee replacement. He is a reviewer of current research for the Bone and Joint Journal, The Journal of Arthroplasty, and the American Journal of Orthopedics.
Dr. Benjamin McArthur is a fellowship-trained orthopedic surgeon at Washington Orthopaedics & Sports Medicine. His specializations include hip and knee replacement, complex revision hip and knee replacement, and hip preservation surgery. He has published numerous peer-reviewed articles and has presented at national and international events on topics related to hip and knee replacement. He is a reviewer of current research for the Bone and Joint Journal, The Journal of Arthroplasty, and the American Journal of Orthopedics.
Want to know more?
For more information about joint replacement and recovery, email us or request an appointment. Be sure to follow us on Facebook and Twitter as well!
